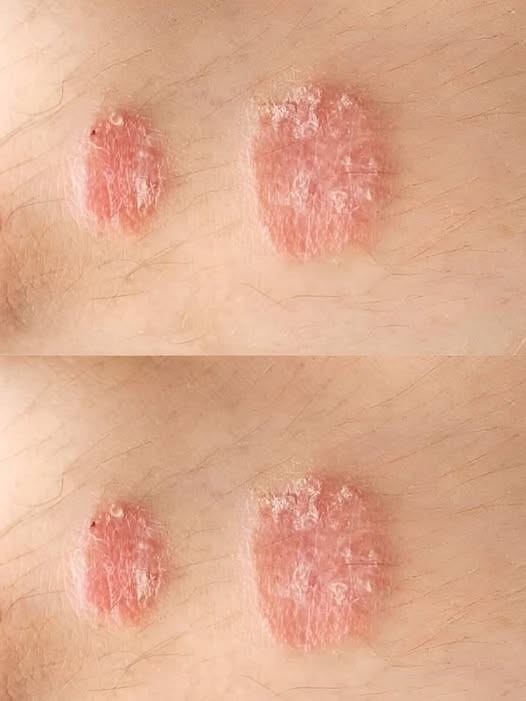
Emotional and Social Considerations
Psoriasis is not just a skin condition—it can affect emotional well-being. Many people experience self-consciousness, anxiety, or depression because of visible skin patches.
Support groups, counseling, and open conversations with healthcare providers can help manage these challenges. Learning to advocate for your own health and educate others about psoriasis can reduce stigma and improve mental well-being.
When to See a Doctor
See a healthcare provider if you experience:
-
Rapidly worsening patches or severe flare-ups
-
Intense pain, itching, or bleeding
-
Signs of infection, such as pus or swelling
-
Emotional distress related to your condition
Early treatment and professional guidance improve symptom management and prevent complications, including psoriatic arthritis or severe skin infections.
Key Takeaways
-
Psoriasis is a chronic, autoimmune skin disease affecting millions worldwide.
-
There is no cure, but symptoms can be managed effectively with medical treatment and lifestyle adjustments.
-
Triggers include stress, infections, medications, and environmental factors.
-
A combination of topical treatments, phototherapy, systemic medications, and healthy habits helps control flare-ups.
-
Emotional support is as important as physical treatment for overall well-being.
Psoriasis may be incurable, but it doesn’t have to define your life. With the right approach, you can reduce flare-ups, relieve discomfort, and maintain confidence in your skin. Awareness, early intervention, and consistent care are key to living fully with psoriasis.